
This is my second speech to NNLM, the Network of the National Library of Medicine. As I said in announcing the first one,
Medical librarians (“medlibs”) have always been a magical resource, to me, because in addition to helping researchers and medicos, they can help ordinary people dig up information they need but don’t know where to find. It’s truly empowering.
I want both the public and medlibs to know how important it is for them to connect. Knowledge is power.
When a new universal truth emerges, you see signs of it all over the place. On March 30 I gave my first speech of how this is playing out (right now) in my life: being an empowered, engaged “e-patient” is helping me once again, as it did 15 years ago with my life-threatening cancer. This time it’s a vision-threatening condition: glaucoma, a leading cause of blindness. Not cool.
As regular readers of this blog know, I got glaucoma a year ago after routine eye surgery went wrong and other complications unfolded. As I blogged in my previous post, when the NNLM (Network of the National Library of Medicine) invited me to speak for them again, it was an opportunity to revisit what I’d taught before, applying it this time to a completely new field: my need to become empowered and engaged in a new field, to avoid blindness.
The story is in this 34 minute speech. (Email subscribers, click the headline above to come online.)
I describe how when this news hit, I went through the emotional reactions we all do at diagnosis (anger, fear, confusion), and then got to work: “pulled up my big girl pants” and started educating myself. I share my discovery of a world of things I’d never known about eyes – and a boatload that patients talk about and most doctor visits don’t. As you’ll hear, it took me six months to find a great patient community (FitEyes.com). From them, and from my own research, I learned many things that matter to patients and aren’t in patient education pamphlets. Examples:
- Statistics on how often my surgical problems happen
- How to cope with the difficulty of administering eye drops … advice I learned from the patients, not from the doctors
- The lack of any evidence-based methods for how to use eye drops(!) It’s appalling, since eye drops are the only way glaucoma is managed. What the heck – no evidence-based standards??
- A home eye pressure machine I bought (not cheap – a real medical device) that lets me check my eye pressure between visits … in exactly the same way people with diabetes can check their blood sugar at home:
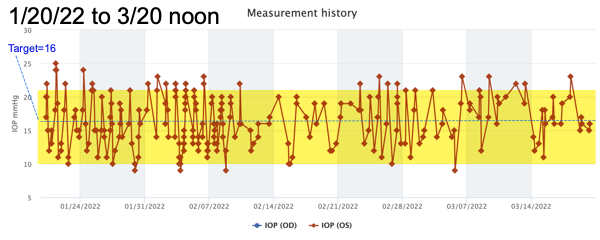
I also note a spectacular thing that happened in my working relationship with my ophthalmologists at OCB, my clinic in Boston: when I brought up the difficulty of using eye drops, my glaucoma specialist (Dr. Theodor Sauer) came back to me with literature links he’d found on the subject – something they hadn’t focused on before. Participatory medicine!
At the end of the talk I shift gears away from eye care, to talk about how patients today are starting to play an active partnership role in clinical research. That’s a lead-in to my next speech, April 19, for Virginia Commonwealth University. Like this NNLM talk, the VCU one is open to the public with free registration.


[…] his blog where he discusses more about his diagnosis and NNLM […]