Response to this on social media has been very strong. Why?
At conferences people are always asking how to comprehend what policy people call “patient experience.” Too often they think it’s things like “Was the food good? Did we smile for you? Was parking easy?” This diagram may help change that.
Have you ever been given instructions by a clinician that are really hard for you to follow? Have you ever thought to yourself, “Don’t they know I have a life? And I have to take care of my sick mother, too, and my car broke down, and…?”
And then for many of us there are all the complications of managing multiple conditions.
Lots of people talk about the burden of a disease, but what about the burden of treatment – when the treatment itself makes life more difficult? How ironic, when the whole point of care was to make life better?
I first heard about this issue from the Mayo Clinic’s Victor Montori when we both spoke last January at Maine Quality Counts. (I blogged his slides and speech video: Careful and Kind Care for our Complex Patients.)
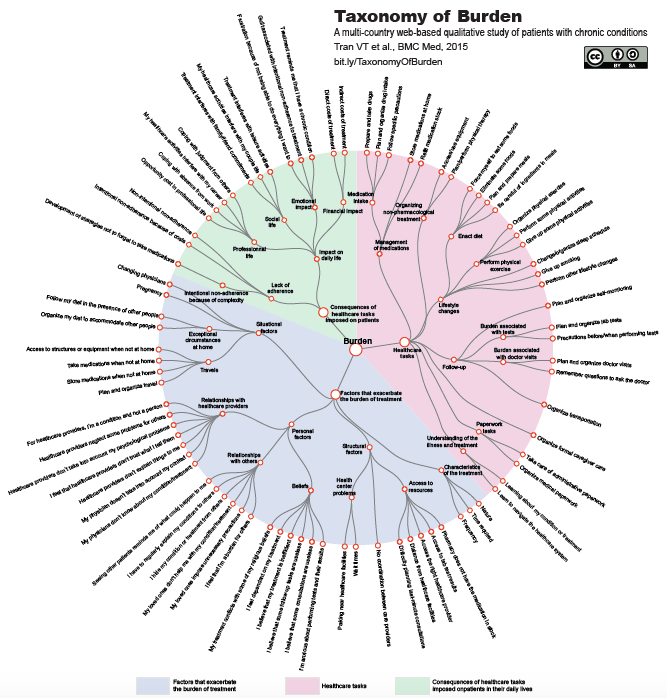
Yesterday I learned about the graphic you see here, which was published last year as part of a paper in the journal BMC Medicine. I love it. At the very center is one item: the word “burden.” Coming out from it are three dots:
- Healthcare tasks: the things you’re told to do.
- Consequences of healthcare tasks imposed on patients. (See above!)
- Factors that worsen the burden of treatment: communication problems, getting to and from the doctor’s office, etc etc.
Then, extending from each, are additional realities: under Tasks are paperwork, understanding the illness, follow-up, rearranging life etc etc; under Consequences are impact on work, financial impact, etc etc; under factors that worsen are the many many things that just plain get in the way of doing the right thing.
The “holy crap” effect
Why do I love this graphic? That whole thing could be printed out as an outline list, many pages long, but that has no “all at once” impact: you browse a list item by item, but this visualizes it all at once, making you realize: “Holy crap! Look at all this!”
I know some absolutely wonderful care professionals – usually nurses, but some great doctors too – who are fabulous about listening for the impact of these challenges on the patient’s life. (Examples include my PCP, Dr. Danny Sands, and of course Victor Montori.) It really takes something for them to add this thinking to their existing burden of work and following regulations. Blessings on all such committed, caring professionals!
Share and share alike:
The diagram is from this article in BMC Medicine: bit.ly/TaxonomyOfBurden, by Viet-Thi Tran , Caroline Barnes, Victor Montori, Bruno Falissard and Philippe Ravaud.
I’m publishing this because I hope it will help us all understand some of the many ways it can be hard to achieve the best of care. You’re welcome to download this, share it freely, take it to your appointments, etc: it’s “Creative Commons Share-Alike with Attribution” – anyone is welcome to reuse it, as long as the credit is carried with it.


There is so much more work to do in this area. Helping clinicians and managers become aware of the work of being a patient and how the way we organize and deliver care can overwhelm the capacity of patients and their families and disrupt their life is a key agenda for transforming care.
We recently started The Patient Revolution organization, an advocacy and action group that plans to transform healthcare by drawing and deploying patient stories. Instead of the industrial and financial version of healthcare, we seek careful and kind patient care (more on this at: patientrevolution.org). To read more about Treatment Burden and Minimally Disruptive Medicine visit MinimallyDisruptiveMedicine.org.
Thanks Dave for disseminating this important work and drawing activism in its direction.
I’d love to see a pediatric version of this study, especially one that pays particular attention to the social context of chronic condition/disability.
The study notes that adults with chronic conditions often face indirect professional consequences. But children with chronic conditions, because they are routinely under the care of non- family member adults, can face social burdens adults do not.
Children too young to self-manage chronic conditions (I am thinking of type 1 diabetes) often face direct discrimination: exclusion from school, child-care facilities, or other programs because responsible adults refuse to provide or supervise routine and even emergency care. While in the U.S. such exclusions are broadly contrary to federal law, enforcement is via an individual complaint mechanism (USDOJ or private lawsuit). Because most schools and programs do not routinely employ full-time nurses, and state laws don’t always explicitly support provision of medical care by lay people in school or childcare settings, legal challenges are likely to be beyond the capacity of most individual families.
Even if undertaken and successful, a legal challenge imposes a considerable additional burden, both financial and potentially social, in the form of resentment from staff or other parents if a school or program unwillingly expends resources to accommodate the child. State child welfare laws, which can construe non-adherence to chronic condition treatment as child abuse, also complicate the burden model.
This is especially true regarding teens with chronic conditions, who must learn independent condition management while their parents may still face criticism (or even investigation by child welfare entities) for poor treatment outcomes. For pediatric patients with chronic conditions, triangulation between doctor/state (mandatory reporting), parent, and patient complicates the medical burden of treatment; triangulation between family, school or other caregiver who may be responsible for care tasks, and patient complicates the social burden of treatment.
What a terrific, concrete, specific, useful comment, Julia. (All, Julia is on Twitter as @JuliaBoss5 and also as @T1DF_advocacy.)
Julia, agreed. There is indisputably an impact. While adults/parents of child/youth w/ health challenges often feel isolation, the kids feel that distance and more. As I recall, the stats on bullying and chronic conditions is pretty scary.
As someone who has lived with the long term effects of cancer treatment for over 20 years, this is an excellent representation of what patients have to go through.
“Careful and kind care for complex patient” what a ground-breaking concept. In my 50 years of treatment as a Type One Diabetic, this has never happened, many times quite the opposite. I love Victor Montori’s work.
I LOVE this. I can’t even begin to explain the sum of this diagram to people most days. They just don’t get how heavy and challenging it is to balance this without a single other issue of life added in. My breaking point is not lower than theirs. I just start closer to it. The dragons I fight are invisible. It doesn’t mean they’re not there.
So, you know you can click to download that (or print this blog post) to show people, right? (Clinicians may find validation in the fact that it’s in a peer reviewed medical journal.)